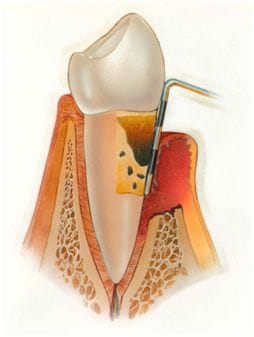
What is Periodontics and What is a Periodontist?
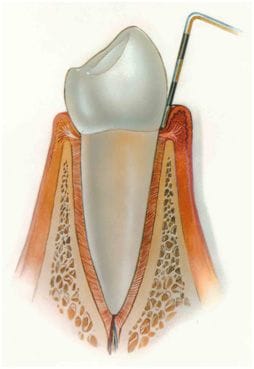
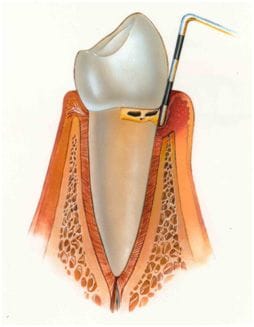
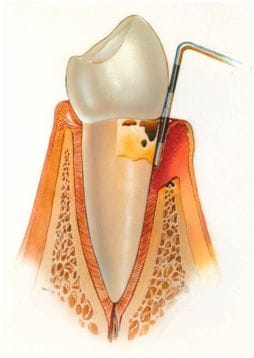
Periodontics is the specialty of dentistry that studies the supporting structures of teeth, diseases, and conditions that affect them. The supporting tissues are known as the periodontium, which includes the gingiva (gums), alveolar bone, cementum, and the periodontal ligament. A periodontist is a fully qualified dentist who has undergone additional University postgraduate training (three years full time), enabling him/her to register in Australia as a Specialist in the field. Their level of expertise allows them to provide a higher level of care in the field of treatment of gum diseases, placement and maintenance of dental implants, and associated surgical procedures.